The single greatest impediment to error prevention in the medical industry is “that we punish people for making mistakes.”
Dr. Lucian Leape
Harvard School of Public Health
Testimony before Congress on Health Care Quality Improvement
 The patient safety movement has embraced as its central thesis that most medical errors are the result of bad systems, not bad people. This thesis has resulted in an evolution to a “no blame” culture. Doing so has encouraged health care providers to report their errors and near misses so that organizations can employ “systems thinking” to understand the underlying “latent conditions” that contribute to errors and to develop programs to focus on identifying and fixing dysfunctional systems.
The patient safety movement has embraced as its central thesis that most medical errors are the result of bad systems, not bad people. This thesis has resulted in an evolution to a “no blame” culture. Doing so has encouraged health care providers to report their errors and near misses so that organizations can employ “systems thinking” to understand the underlying “latent conditions” that contribute to errors and to develop programs to focus on identifying and fixing dysfunctional systems.
Recent data from the U.S. Agency for Healthcare Research and Quality (AHRQ)¹ suggests that this approach is working. The AHRQ has reported that progress in quality and patient safety driven by the Affordable Care Act (ACA) is associated with 1.3 million fewer hospital-acquired conditions and 50,000 fewer inpatient deaths between 2011 and 2013.
While this “blameless” approach is largely correct and is responsible for the field’s evolution to a blameless culture, it needs to be balanced with accountability. Banner Health has adopted a method that the Banner – University Medical Center (UMC) South hospital has been using for years for assessing individual culpability when medical errors occur, it’s called “Just Culture.” The Just Culture philosophy is built upon four foundational elements that permit differentiation of innocent from blameworthy mistakes:
- Individual practitioners should not be held accountable for system failings over which they have no control.
- Just Culture recognizes that many errors represent predictable interactions between human operators and the systems in which they work and recognizes that competent professionals make mistakes.
- Just Culture acknowledges that even competent professionals will develop unhealthy norms (shortcuts, workarounds, and “routine rule violations”).
- A Just Culture has zero tolerance for reckless behavior.
Going forward, when adverse events associated with patient harm are reported by anyone in the institution or when adverse outcomes are detected using predefined triggers — e.g., inpatient deaths, post-procedure complications, using too much contrast in the cath lab, late detection of sepsis — a defined algorithm (see graphic below²) will be used to assess if the individuals involved were in some way culpable.
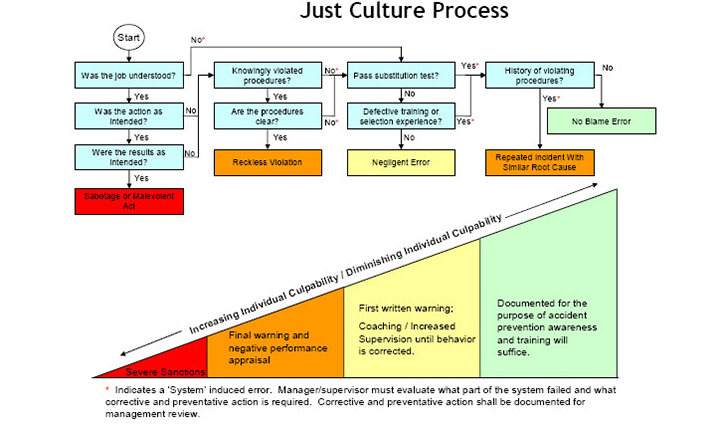 When an event occurs here at the Banner UMC Tucson and South campuses — our main teaching hospital facilities, the case will be reviewed by the Peer Review Committee members. They will review the case in detail, apply the Just Culture Algorithm and provide you with feedback.
When an event occurs here at the Banner UMC Tucson and South campuses — our main teaching hospital facilities, the case will be reviewed by the Peer Review Committee members. They will review the case in detail, apply the Just Culture Algorithm and provide you with feedback.
The question this algorithm poses is if the error was the result of defective systems and if the same would have happened in the hands of any provider in the same circumstance. Some errors are the result of reckless acts or worse. I hope that all would agree that these errors warrant disciplinary action. Finding a balance between the extremes of punishment and blamelessness and applying standards uniformly to everyone is the goal of Just Culture.
In the end, though, it is all about creating an atmosphere and process where the best care can be provided consistently for the many patients that entrust their health into our capable hands.
- Eliminating CLABSI, A National Patient Safety Imperative: Final Report. January 2013. Agency for Healthcare Research and Quality, Rockville, MD. http://www.ahrq.gov/professionals/quality-patient-safety/cusp/clabsi-final/index.html
- Safety Management System Toolkit. September 2007. Joint Helicopter Safety Implementation Team of the International Helicopter Safety Team, Montreal, Canada, (see page 29). http://www.ihst.org/Portals/54/SMS-Toolkit.pdf
This blog topic was originally posted March 15, 2016.

