Led by Monica Kraft, MD, at the University of Arizona College of Medicine – Tucson, researchers will use the National Institutes of Health grant to conduct a five-year study, “Dysfunction of Innate Immunity in Asthma,” to investigate the interrelationship of genetic mediators to reduce lung inflammation and attacks in asthma patients.
 About 25 million people in the United States—7 million of them children—suffer from asthma. A five-year, $7 million National Institutes of Health grant awarded recently to Monica Kraft, MD, an internationally renowned physician-scientist who specializes in translational asthma research at the University of Arizona College of Medicine – Tucson and the UA Health Sciences’ Asthma and Airways Diseases Research Center, will seek a better understanding of mediators that help control lung inflammation and improved therapies to reduce severe attacks in those with asthma.
About 25 million people in the United States—7 million of them children—suffer from asthma. A five-year, $7 million National Institutes of Health grant awarded recently to Monica Kraft, MD, an internationally renowned physician-scientist who specializes in translational asthma research at the University of Arizona College of Medicine – Tucson and the UA Health Sciences’ Asthma and Airways Diseases Research Center, will seek a better understanding of mediators that help control lung inflammation and improved therapies to reduce severe attacks in those with asthma.
Funded through the National Institute of Allergy and Infectious Diseases (NIAID), the grant will support a research study, “Dysfunction of Innate Immunity in Asthma,” with three projects, including analysis of human samples of people with asthma and investigation of genetic markers related to dysfunctional immune response mechanisms in asthma. The goal is to develop a better understanding of those mechanisms and refine novel therapies to moderate or eliminate asthma attacks and enable asthma sufferers to breathe easier.
 Dr. Julie Ledford and Akarsh Manne (left), an associate scientific investigator for Dr. Kraft, discuss results from a recent genetic analysis of samples in her lab in the Keating Building of the UA BIO5 Institute.
Dr. Julie Ledford and Akarsh Manne (left), an associate scientific investigator for Dr. Kraft, discuss results from a recent genetic analysis of samples in her lab in the Keating Building of the UA BIO5 Institute.
Analysis will focus on dysfunctional single nucleotide polymorphisms (SNPs or “snips”) of surfactant protein A (SP-A), a lipid constituent of surfactant known as POPG (palmitoyl-oleoyl-phosphatidylglycerol) and Toll-like receptor interacting protein (Tollip). Surfactant helps to open up aveolar sacs in the lungs and change surface tension so lungs can expand. SP-A, POPG and Tollip act as mediators, signaling synergistically which foreign irritants or conditions in the lungs to attack or not. Each perform critical negative regulatory functions interacting cooperatively to offer protection from allergic inflammation and viral exacerbations of asthma—but, when impaired, cause more acute reactions in asthma sufferers.
“We’ll look at how certain airway cells handle infectious agents in the setting of allergic inflammation in asthma. We’ve found, in humans, not all SP-A is created equal. The same holds true for Tollip. Depending on the genetics of your SP-A or Tollip, their function can be impaired. So, if you have these impaired or dysfunctional aspects of host defense and suffer from asthma, the combination can be very detrimental—leading to more allergic inflammation and asthma attacks,” Dr. Kraft said.
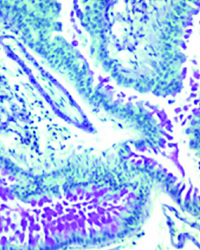 Transmission electron microscope image (on right) of a thin section of the alveolar sac region of the lung. The cell shown has vesicles that contain surfactant, a macroaggregate of phosolipids and proteins that help with breathing.
Transmission electron microscope image (on right) of a thin section of the alveolar sac region of the lung. The cell shown has vesicles that contain surfactant, a macroaggregate of phosolipids and proteins that help with breathing.
“UAHS has some of the best minds in the world working to treat and cure asthma, and this grant from NIH further strengthens the research under way at the UAHS Asthma and Airway Diseases Research Center,” said UA President Ann Weaver Hart. “We are incredibly proud of this work and the good outcomes it will help create for patients.”
“It also dovetails well into the mission of the recently funded NIH Precision Medicine Initiative® Cohort Program, which includes UAHS, to improve prevention and treatment of disease based on individual needs and diverse populations,” said Joe G.N. “Skip” Garcia, MD, UA senior vice president for health sciences, the Dr. Merlin K. DuVal Professor of Medicine and an elected member of the prestigious National Academy of Medicine.
Study participants will be recruited through the UAHS Asthma and Airway Diseases Research Center, with assistance on collecting health data and biological specimens from allergist Tara Carr, MD, and pulmonologist Cristine Berry, MD, MHS, both UA assistant professors. For SP-A lab analysis, Dr. Kraft will work with Julie Ledford, PhD, a UA assistant professor of medicine and immunobiology, who also has worked with her to develop a therapeutic treatment involving small functional peptides of SP-A to correct function of a genetic variant in asthmatics. Two other projects—analysis of the lipid POPG and protein Tollip—will be coordinated by Hong Wei Chu, MD, and Dennis R. Voelker, PhD, of National Jewish Health, an academic medical research facility associated with the University of Colorado – Denver.
Of the genetics of the three signaling pathways—SP-A, POPG and Tollip, Dr. Ledford said, “There are very similar things that they do, but we don’t know a lot about their interaction together. What we have to figure out first is, for these people with this Tollip dysfunctional SNP, do they also have the SP-A dysfunctional SNP? We know people with these SNPs are worse in both cases, but we don’t know if there’s a propensity for them to have both at the same time. We need to find out if that’s the case, how to treat those people better and gain a better understanding of the mechanisms of potential overlap in function and protein regulation.”
Drs. Ledford, Chu and Voelker are longtime collaborators with Dr. Kraft when she was at Duke University and the University of Colorado before joining the UA in 2014 as chair of the UA Department of Medicine—the largest department at the College of Medicine – Tucson—and the Robert and Irene Flinn Endowed Chair of Medicine. A past president of the American Thoracic Society, Dr. Kraft also has been a key global investigator into the causes and potential cures for asthma.
Dr. Ledford said, “We are working on a particular therapeutic that would help people who have surfactant dysfunction in asthma, so it’s just a really great opportunity for us to move our research forward and be able to work with these specialists at National Jewish to continue our program that we’ve had together for so long.”
The study is part of NIAID’s U19 Cooperative Research Program, which involves about a dozen Asthma and Allergic Diseases Cooperative Research Centers (AADCRCs) across the country—of which the UA is the newest.
 That aspect of inclusion in a broader mission through the NIAID’s AADCRC group excited Dr. Kraft (pictured on the right in clinic recently with an asthma patient for an initial evaluation).
That aspect of inclusion in a broader mission through the NIAID’s AADCRC group excited Dr. Kraft (pictured on the right in clinic recently with an asthma patient for an initial evaluation).
“Even though we have an independent U-19 project, we also collaborate with other centers that are part of this network. We meet in person as well as through conference calls—and when there’s an opportunity to do additional projects with pooled funds, you have to apply. It’s not just independent, meaning it’s not just us. We’re all over the world. We’re accountable to the network,” she said, pointing out that pooled resources and data allow for potential advances to be exponential.
This research is supported by the NIH under award number 1 U19AI125357-01.
NEWS MEDIA: For additional information or to interview Dr. Kraft, please contact David Mogollón, 520-626-1137, dmogollon@deptofmed.arizona.edu — b-roll and photos available.
ALSO SEE:
"$7M NIH Asthma Grant to UA College of Medicine – Tucson" | UANews | Posted Aug. 12, 2016
"Amish Farms May Protect Children Against Asthma" | UANews | Posted Aug. 4, 2016
"UA Researchers Link Genetic Variation in Pulmonary Protein to Respiratory Disease" | Posted Dec. 22, 2015


