A member of the National Cancer Institute Head and Neck Cancer Steering Committee and a former Tucsonan, Julie E. Bauman, MD, MPH, joins the UA College of Medicine – Tucson faculty as professor and chief of the Division of Hematology and Oncology in the Department of Medicine and the UA Cancer Center.
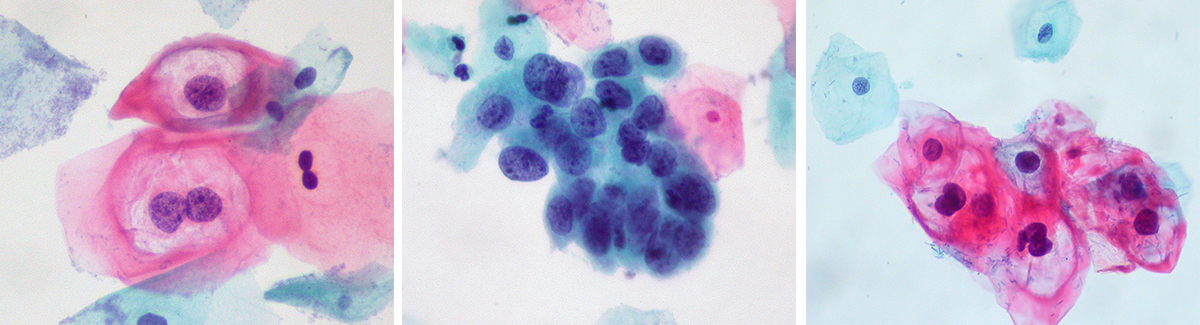
Reducing throat cancer caused by human papillomavirus (HPV) among men is one focus of Dr. Bauman’s research, resulting in her advocacy for teens of both sexes to get the HPV vaccine before they become sexually active. Pictured—left to right—a low-grade squamous intraepithelial lesion, with HPV effect; a high-grade squamous intraepithelial lesion, also known as high-grade dysplasia; and a group of HPV-infected koilocytes on the bottom right accompanied by two normal intermediate squamous cells at the top and left.
 Julie E. Bauman, MD, MPH, is no stranger to Tucson.
Julie E. Bauman, MD, MPH, is no stranger to Tucson.
The renowned head and neck cancer specialist and physician-scientist, who starts Sept. 1 as a professor of medicine and the new chief of the Division of Hematology and Oncology at the University of Arizona College of Medicine – Tucson and the UA Cancer Center, is a 1985 graduate of Salpointe Catholic High School.
“For me, it’s a homecoming,” Dr. Bauman said. “I was raised in Tucson. The Southwest is my home, my community and my culture. I did my junior faculty experience nearby at the University of New Mexico Cancer Center and returning to a leadership position at a Southwestern cancer center in an underserved state seems like the natural step for me in terms of my service.”
She spent the past four years in Pittsburgh, where she was associate professor of medicine at the University of Pittsburgh Cancer Institute (UPCI), co-leader of the UPCI Head and Neck Cancer Program, director of its Head and Neck and Thyroid Cancer Sections, and co-director of the Head and Neck Cancer Center of Excellence at the University of Pittsburgh Medical Center. She has been a member of the National Cancer Institute (NCI) Head and Neck Cancer Steering Committee, and currently chairs the Immunotherapy Working Group for the NCI Recurrent/Metastatic Task Force. Her research focuses on design of biomarker-driven, early-phase clinical trials to prevent and improve survival in head and neck cancer, a disfiguring and devastating disease.
Her new division is part of the UA Department of Medicine—the largest department in the College of Medicine – Tucson—and functions largely through the UA Cancer Center, which had its designation as the only Comprehensive Cancer Center based in Arizona renewed recently by the National Cancer Institute (NCI) along with the award of a five-year, $17.6 million support grant.
 “I am so pleased to welcome Julie,” said department Chair Monica Kraft, MD, UA professor of medicine and the Robert and Irene Flinn Endowed Chair of Medicine. “She has an outstanding track record of research and clinical training, and will lead our hematology/oncology division to greatness. Her work not only aligns very well with strengths at the University of Arizona, but she brings new therapeutic programs with her as well.”
“I am so pleased to welcome Julie,” said department Chair Monica Kraft, MD, UA professor of medicine and the Robert and Irene Flinn Endowed Chair of Medicine. “She has an outstanding track record of research and clinical training, and will lead our hematology/oncology division to greatness. Her work not only aligns very well with strengths at the University of Arizona, but she brings new therapeutic programs with her as well.”
Dr. Bauman said she’s delighted to be working with UA Cancer Center Director Andrew S. Kraft, MD, a professor of medicine, UA Health Sciences associate vice president for oncology programs and senior associate dean for translational research and the Sydney E. Salmon Endowed Chair at the UA College of Medicine – Tucson.
“We’re excited by the strengths—research, clinical and advocacy—that Dr. Bauman brings to the position,” said Dr. Kraft. “They complement and augment very well many things we are already doing at the UA Cancer Center.”
 Also eager for her arrival is Steven J. Wang, MD, interim chair of the UA Department of Otolaryngology — Head and Neck Surgery.
Also eager for her arrival is Steven J. Wang, MD, interim chair of the UA Department of Otolaryngology — Head and Neck Surgery.
“It is exciting to have a distinguished expert in head and neck medical oncology to lead the hematology/oncology division and to join our multidisciplinary head and neck cancer program at the UA Cancer Center,” Dr. Wang said. “I look forward to working with Dr. Bauman to be able to offer unique access to innovative clinical trials and cutting-edge precision treatments for head and neck cancer patients from across Arizona and the Southwest.”
Dr. Bauman’s goal for the division is to work with faculty and staff to design and conduct rigorous clinical trials that bring cutting-edge scientific laboratory findings into the prevention and treatment of cancer. Her three areas of research have focused on “green chemoprevention”—using plants or their simple extracts to help the body detoxify carcinogens, battling the epidemic of throat cancer caused by human papillomavirus (HPV), and the emerging field of immuno-oncology—novel treatments that activate the immune system to fight cancer.
“Head and neck cancer fundamentally affects critical human functions—speaking, breathing, facial expressions, swallowing, eating. So, head and neck cancer and its treatments, including chemotherapy, radiation and surgery, can be disfiguring and permanently alter those functions,” Dr. Bauman said.
“The lessons I’ve learned in caring for people with this difficult disease apply across the spectrum of cancer—not only do we need to heal the patient, we also must strive to prevent cancer, and when we cannot, minimize the lasting effects of treatment on the whole person.”
Green Chemoprevention
 The first step is to prevent head and neck cancer in the first place, which draws on one area of her research—green chemoprevention. This includes reducing exposure to environmental carcinogens like tobacco and alcohol, but also means generally incorporating healthier eating habits—more fruits and vegetables—into one’s diet. For clinical purposes specifically, it involves use of whole plants or their simple extracts to prevent cancer via their detoxifying properties.
The first step is to prevent head and neck cancer in the first place, which draws on one area of her research—green chemoprevention. This includes reducing exposure to environmental carcinogens like tobacco and alcohol, but also means generally incorporating healthier eating habits—more fruits and vegetables—into one’s diet. For clinical purposes specifically, it involves use of whole plants or their simple extracts to prevent cancer via their detoxifying properties.
Cruciferous vegetables, such as broccoli (right), contain a compound in high concentrations—sulforaphane—that helps the body metabolize and excrete cancer-causing toxins.
In this regard, Dr. Bauman and her collaborators focus on green, leafy cruciferous vegetables like kale, cauliflower, Brussel sprouts and broccoli and a compound, or phytochemical, found in high concentrations in them, sulforaphane. A paper she co-wrote on the topic appeared in the June issue of the journal Cancer Prevention Research, “Prevention of Carcinogen-Induced Oral Cancer by Sulforaphane.”
It involved use of beverages derived from broccoli sprout extract to help the body get rid of air pollution toxins. Another colleague, she said, “showed that in a population in China, where air pollution rates are so high people are inevitably exposed, this compound helps their bodies metabolize and excrete them” more efficiently.
Human Papillomavirus
Over the past decade, HPV, the same virus that causes cervical cancer in women, has caused a growing epidemic of throat cancer, particularly among men in their peak productive years of age 40 to 60.
“I am focused on understanding the biology of HPV and how the virus interacts with DNA to cause cancer. I have a grant looking at a specific mutation in the PIK3CA gene, which is abnormal in about 60 percent of HPV-related throat cancers,” Dr. Bauman said.
She points out drug therapies to target this gene exist that are being improved, but that the best way to avoid HPV-related throat cancer is for both boys and girls to be vaccinated prior to becoming sexually active.
“In this realm of prevention, I do advocacy work around the HPV vaccination where it works to prevent people from contracting HPV infections in the first place,” she added. “And it’s actually indicated for both boys and girls by the Food and Drug Administration. Once you have an established infection or cancer, it’s too late. The vaccine doesn’t treat infection or cancer, it only prevents it.”
Immuno-Oncology
Here, Dr. Bauman refers to “a whole new world” of medications that activate the immune system to fight cancer, whether by themselves, or in combination with radiation or chemotherapy.
She used as an example the first of these to be approved by the FDA—just last week—for head and neck cancer, pembrolizumab (Keytruda®)—an antibody that reeducates or reawakens killer T-cells to fight cancer. The T-cells have been sedated or exhausted—hypnotized, if you will—by the cancer to hide from the immune system. The combination therapy helps T-cells see the cancer and destroy it.
“That is the promise,” she said. “And the field is transforming before our very eyes.”
Her involvement includes early-phase clinical trials to bring these exciting therapies to patients with cancer for the first time, and randomized trials to bring them to market.
The Long Road Back
Before moving to Pittsburgh in 2012, Dr. Bauman was an assistant professor in the Division of Hematology and Oncology at the University of New Mexico and UNM Cancer Center in Albuquerque. She also served as chair of UNM’s head and neck cancer and lung cancer working groups. And she was its principal investigator with the Eastern Cooperative Oncology Group (ECOG)—one of the first publicly funded cooperative research groups to perform multi-center clinical trials for cancer studies.
She completed her fellowship in medical oncology at the University of Washington’s Fred Hutchinson Cancer Research Center, where she was chief fellow and later an assistant professor of medicine. She completed her residency in internal medicine at the University of Utah and earned her medical and master’s in public health degrees from Tufts University. Her undergraduate degree in psychology is from Eastern Michigan University.
------------------------------------------------------
NEWS MEDIA: For additional information or to interview Dr. Bauman, please contact David Mogollón, 520-626-1137, dmogollon@deptofmed.arizona.edu

