 Monica Kraft, MD, professor and chair of the University of Arizona Department of Medicine, the Robert and Irene Flinn Endowed Chair of Medicine, and deputy director of the UA Health Sciences Asthma and Airway Disease Research Center, has been named to the National Heart, Lung, and Blood Advisory Council.
Monica Kraft, MD, professor and chair of the University of Arizona Department of Medicine, the Robert and Irene Flinn Endowed Chair of Medicine, and deputy director of the UA Health Sciences Asthma and Airway Disease Research Center, has been named to the National Heart, Lung, and Blood Advisory Council.
 “It is an honor to be chosen for such an important and prestigious position,” Dr. Kraft said. “I am indebted to the NIH for supporting me all these years so I’m happy to give back any way I can.”
“It is an honor to be chosen for such an important and prestigious position,” Dr. Kraft said. “I am indebted to the NIH for supporting me all these years so I’m happy to give back any way I can.”
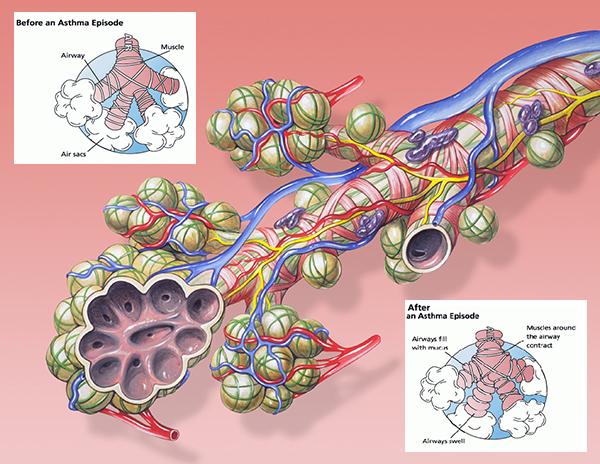
Illustration (right) of pulmonary aveolus, or tiny air sacs in the lungs, and how they’re affected by asthma attacks. Dr. Kraft’s research has been instrumental in helping understand dysfunctional inflammation in severe asthma in adults and how to better manage it to reduce the severity and frequency of attacks. (Image: Olve Utne/FDA)
The council advises the secretary of the U.S. Department of Health and Human Services (DHHS), the DHHS assistant secretary for health, the director of the National Institutes of Health (NIH), and the director of the National Heart, Lung, and Blood Institute (NHLBI) on matters related to the cause, prevention, diagnosis and treatment of heart, blood vessel, lung and blood diseases; use of blood and blood products and management of blood resources; and sleep disorders.
 The council considers applications for research and research training grants and cooperative agreements and recommends funding for those applications that show promise of making valuable contributions to human knowledge. It also may make recommendations to the NHLBI director about research conducted at the institute. The council meets four times a year—usually winter, spring and two meetings in the fall. Minutes of the most recent meetings are available online to read or download.
The council considers applications for research and research training grants and cooperative agreements and recommends funding for those applications that show promise of making valuable contributions to human knowledge. It also may make recommendations to the NHLBI director about research conducted at the institute. The council meets four times a year—usually winter, spring and two meetings in the fall. Minutes of the most recent meetings are available online to read or download.
Dr. Kraft’s term runs from July 23, 2018, through Oct. 31, 2021, although she attended her first meeting of the council as an ad hoc member June 12. That meeting included updates from NHLBI Director Gary Gibbons, MD, and All of Us℠ Research Program Director Eric Dishman on the growing potential that precision medicine offers and how the institute is collaborating with the program.
Dr. Kraft, a renowned physicians-scientist who first received NIH research funding in 1995, focuses her work on precision medicine therapies to treat severe asthma. As a principal investigator, she currently is in the third year of a 5-year, $7.02 million grant from the National Institute of Allergy and Infectious Diseases, another NIH institute, to study “Dysfunction of Innate Immunity in Asthma” (NIAID/NIH Award No. U19AI125357) and the first year of a 6-year, $2.42 million grant from NHLBI with UA co-principal investigator Eugene Bleecker, MD, for participation in the PrecISE Network, a national research cohort involved in a study focused on “Precision Interventions for Severe and/or Exacerbation Prone Asthma” (NHLBI/NIH Award No. UG1HL139054).
 Drs. Monica Kraft and Tara Carr, an allergist in the UA Division of Pulmonary, Allergy, Critical Care and Sleep Medicine, co-authored a paper on “Use of Biomarkers to Identify Phenotypes and Endotypes of Severe Asthma” that appears in the July 27 issue (see cover at left) of the Annals of Allergy, Asthma & Immunology.
Drs. Monica Kraft and Tara Carr, an allergist in the UA Division of Pulmonary, Allergy, Critical Care and Sleep Medicine, co-authored a paper on “Use of Biomarkers to Identify Phenotypes and Endotypes of Severe Asthma” that appears in the July 27 issue (see cover at left) of the Annals of Allergy, Asthma & Immunology.
The PrecISE study, which is expected to split as much as $100 million in additional project funding later this year, aims to identify more effective treatments for severe asthma which affects nearly 10 percent of people worldwide and remains poorly controlled for many patients. The study is an innovative clinical trial that will support a personalized medicine approach to identifying therapies tailored to an individual’s disease and treatment history.
Dr. Kraft wasn’t the only UA Wildcat at the June advisory council meeting in Washington, D.C., though.
 “(UA President) Dr. Robert Robbins is a current member, and Dr. Fernando Martinez (director, UAHS Asthma and Airway Disease Research Center) has just completed his term,” said Laura K. Moen, PhD, director of the NHLBI’s Division of Extramural Research Activities, which works closely with the council. “Therefore, this advisory council is well represented by University of Arizona faculty!”
“(UA President) Dr. Robert Robbins is a current member, and Dr. Fernando Martinez (director, UAHS Asthma and Airway Disease Research Center) has just completed his term,” said Laura K. Moen, PhD, director of the NHLBI’s Division of Extramural Research Activities, which works closely with the council. “Therefore, this advisory council is well represented by University of Arizona faculty!”
The group will meet again by teleconference for grant reviews later this month, then meets in person in September and October in the nation’s capital.
Dr. Kraft joined the UA College of Medicine – Tucson faculty in 2014, coming from Duke University in Durham, N.C., where she served as chief of the Division of Pulmonary, Allergy and Critical Care and founding director of the Duke Asthma, Allergy and Airway Center. Before that, she was director of the Carl and Hazel Felt Laboratory in Adult Asthma Research and as medical director of the pulmonology physiology unit at the National Jewish Medical and Research Center in Denver. Among her many honors, she received the Presidential Early Career Award for Scientists and Engineers, awarded at the White House in 2000, and served as president of the American Thoracic Society in 2012-13.
She also has written more than 175 publications in the areas of adult asthma, the role of infection in asthma and the role of the distal lung in asthma and airway remodeling.
Dr. Kraft’s primary research colleagues at the UA include:
 Julie Ledford, PhD, assistant professor of medicine and immunobiology and, like Dr. Kraft, a member of the UA BIO5 Institute which hosts their labs (a long-time collaborator with Dr. Kraft both at Duke and the UA, Dr. Ledford is co-investigator with her on several studies, including the NIAID grant which seeks to further develop a peptide as therapy to counter a dysfunctional protein, SP-A, in asthma sufferers); and
Julie Ledford, PhD, assistant professor of medicine and immunobiology and, like Dr. Kraft, a member of the UA BIO5 Institute which hosts their labs (a long-time collaborator with Dr. Kraft both at Duke and the UA, Dr. Ledford is co-investigator with her on several studies, including the NIAID grant which seeks to further develop a peptide as therapy to counter a dysfunctional protein, SP-A, in asthma sufferers); and- Eugene R. Bleecker, MD, and Deborah A. Meyers, PhD, professors of medicine, co-chiefs of the Division of Genetics, Genomics and Precision Medicine, and co-directors of the Division of Pharmacogenomics in the UAHS Center for Applied Genetics and Genomic Medicine (Dr. Bleecker, who Dr. Kraft recruited to the UA with Dr. Meyers from Wake Forest University, is co-principal investigator with Dr. Kraft on the PrecISE Network study; last fall, the FDA also approved a drug he led clinical trials on for severe asthma patients age 12 or older);
- Stefano Guerra, MD, PhD, MPH, professor of medicine and public health, the Henry E. Dahlberg Chair in Asthma Research, epidemiology unit director at the UAHS Asthma and Airway Disease Research Center, and a BIO5 member (Drs. Kraft and Ledford are among co-investigators on a $3.6 million NIAID grant Dr. Guerra won last fall that seeks to halt persistence of asthma into adulthood), and
- Tara F. Carr, MD, associate professor of medicine and surgery, medical director of the Adult Allergy Program, and director, Allergy and Immunology Fellowship (Dr. Carr serves as a co-investigator on studies by Dr. Kraft and Dr. Guerra to collect health data and biological specimens).
ALSO SEE:
“UA’s Dr. Monica Kraft Receives Distinguished Achievement Award from American Thoracic Society” | Posted May 23, 2018
“FDA Approval for New Severe Asthma Therapy Advanced by Dr. Bleecker’s Research” | Posted Feb. 9, 2018
"Stopping Asthma in Childhood, Goal of $3.6M UA-Led International Consortium Funded by NIH" | Posted Jan. 24, 2018
“Dr. Monica Kraft Named Researcher of the Year by American College of Physicians’ Arizona Chapter” | Posted Oct. 11, 2017
“Drs. Kraft, Ledford Study Finds Molecular Reason for Poor Symptom Control in Obese Asthmatics” | Posted July 14, 2017
"Asthma Research Gets Spotlight in Arizona Republic Op-Ed by UA Senior VPs" | Posted June 15, 2017
“Dr. Monica Kraft Named Fellow in Executive Leadership Program for Women in Academic Medicine” | Posted June 8, 2017
“Department of Medicine Chair Named Fellow of the European Respiratory Society” | Posted June 1, 2017
“DOM Chair’s Senate Testimony at Odds with ADEQ Chief on Relaxing Air Quality Standards” | Posted May 25, 2017
“Dr. Monica Kraft, 11 Other UAHS Investigators Secure ABRC Grant Awards Worth Nearly $6M” | Posted March 6, 2017
“$7 Million NIH Grant Aims at Helping Asthma Sufferers Better Control Attacks, Breathe Easier” | Posted Aug. 11, 2016
“UA Researchers Link Genetic Variation in Pulmonary Protein to Respiratory Disease” | Posted Dec. 12, 2015

